[ad_1]
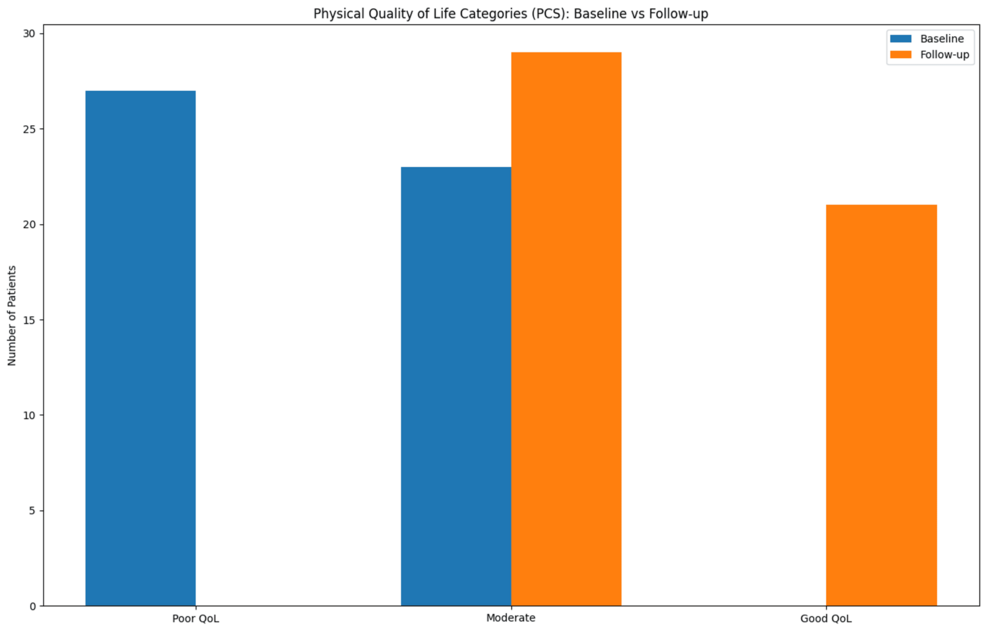
After glucose control and weight loss, GLP-1 drugs are now emerging as potential heart medicines with recent global trials showing they can lower chances of heart attacks and strokes in high-risk patients. In India, where diabetes, obesity, and premature heart disease frequently overlap, cardiologists are increasingly discussing these drugs with patients. Dr Aftab Khan, consultant cardiologist at Apollo Multispeciality Hospitals, Kolkata, tells Umesh Isalkar which patients should consider these drugs first, and why they can complement but not replace proven therapies and lifestyle changes.Why are cardiologists now calling GLP-1 receptor agonists like semaglutide and tirzepatide heart medicines? What changed?Earlier, they were used mainly to control blood sugar and help with weight loss. But over the last few years, large international trials have shown GLP-1 drugs reduce major cardiovascular events such as heart attacks, strokes and heart failure deaths in high-risk patients. For cardiologists, that changes everything. A drug that lowers weight, improves diabetes control, reduces inflammation and lowers cardiovascular risk is no longer just a metabolic drug. It becomes heart risk reduction therapy.The SOUL trial is being described as a landmark study for cardiovascular outcomes in high-risk diabetes patients. What did it prove and why is it significant for patients in India?The SOUL (semaglutide cardiovascular outcomes) trial showed that oral semaglutides significantly reduced heart attacks, strokes and cardiovascular death in people with type 2 diabetes who were already at high cardiovascular risk. This confirms that even the tablet form, not just the injectable version, can protect the heart. For countries like India, where injections can be less acceptable or accessible, an effective oral option makes treatment easier and potentially more scalable. As cardiologists, we believe SOUL trial benefits are very likely to apply to Indian patients, especially since Indians often develop diabetes, obesity, and heart disease at younger ages and lower BMI levels.Studies and the STEP-HFpEF trials suggest symptom and functional improvement with semaglutide in obesity-related heart failure. In practical terms, what changes for a patient?For patients with HFpEF (a form of heart failure in which the left ventricle is stiff and does not fill up fully) linked to obesity, the improvements are quite practical. Patients in trials reported less breathlessness, better ability to walk or exercise, improved quality of life scores, weight loss, and better functional capacity. In simple terms, many patients feel less fatigued, can walk longer distances and perform daily activities more comfortably.
Chronic kidney disease is often silent in Indian diabetics and overlaps with heart disease. How strong is the evidence that GLP-1 drugs protect the kidneys along with the heart?Studies have shown that GLP-1 drugs can slow down worsening kidney function, lower protein leakage in urine and reduce cardiovascular complications in patients with kidney disease. While another class of drugs (SGLT2 inhibitors) currently has stronger kidney-specific evidence, GLP-1 drugs appear to provide additional kidney protection, especially in patients with diabetes and obesity.Which categories of Indian patients should actively discuss GLP-1 drugs with their cardiologist? The first ones should be people with type 2 diabetes who already have established cardiovascular disease — either a prior heart attack, a stent procedure, or a stroke because they remain at high risk of future cardiac events. Overweight or obese individuals with diabetes and high cardiovascular risk are another key group, as these drugs can improve overall metabolic health. Patients with obesity-related heart failure, particularly HFpEF, who experience symptoms like breathlessness and reduced exercise capacity, may also benefit as emerging evidence suggests these therapies can improve symptoms and quality of life.Who should avoid them or exercise caution before use? These drugs should be used cautiously or avoided in patients with a history of pancreatitis, those with certain rare thyroid cancers (such as medullary thyroid carcinoma), patients with severe gastrointestinal disorders, and pregnant or breastfeeding women. A doctor should always evaluate the patient individually before starting therapy.How long should one be on therapy? Are these lifelong drugs like statins?In most cases, these drugs are long-term therapies, similar to statins or blood-pressure medicines. If the medication is stopped, weight and metabolic risk factors often return, so the benefits may diminish. For high-risk patients, cardiologists usually consider them part of long-term risk management.If a patient stops the drug after weight loss, does cardiovascular risk rebound?Regaining weight is common after stopping the medication. When weight and metabolic risk factors return, cardiovascular risk can also rise again. This is why doctors emphasise that these drugs should be used along with lifestyle changes, not as a temporary shortcut.These drugs are expensive and increasingly used off-label for cosmetic weight loss. In India, where access is unequal, who should get priority?From a public health perspective, priority should go to patients with clear medical benefit, such as diabetics with existing cardiovascular disease, high-risk diabetics with multiple risk factors, and those with obesity-related heart failure. Using them purely for cosmetic weight loss while high-risk patients cannot access those, raises ethical and healthcare equity concerns.Is there a danger that patients may stop statins, BP medicines, or lifestyle measures thinking GLP-1 is a ‘magic bullet’?Yes, that is a real concern. GLP-1 drugs are not a substitute for proven therapies. Patients still need statins for cholesterol, blood pressure control, a healthy diet, exercise, weight management and diabetes control. Think of GLP-1 therapy as an additional tool in the cardiovascular prevention toolbox, not a replacement for the basics. Medications cannot fix a bad lifestyle.
[ad_2]