A new RNA-based therapy developed at Columbia University could help the heart repair itself after a heart attack without invasive surgery.

After a heart attack, it is possible for cardiologists to reopen blocked vessels and restart blood flow but the muscle cells that die during this process are lost permanently. Now in a new study, researchers at Columbia University have developed a novel RNA therapy that may help the heart repair itself by enhancing its natural healing mechanisms.
“The heart is one of the organs with the least ability to regenerate,” said Ke Cheng, Alan L Kaganov Professor of Biomedical Engineering at Columbia Engineering. “The spontaneous regeneration power is very, very limited.”
Heart repair without surgery
Cheng and his colleagues designed RNA-lipid nanoparticles that instruct muscle cells in the arm or thigh to produce a molecule called pro-ANP. This inactive precursor circulates through the bloodstream until it reaches the heart, where an enzyme called Corin converts it into the active hormone atrial natriuretic peptide (ANP) which promotes healing.
“You don’t have to open the chest or send a wire to the heart to deliver this drug,” said Cheng. “In principle all the clinician needs to do is to inject the particles into the arm.”
Torsten Vahl, a co-author and cardiologist at Columbia University Irving Medical Center/New York-Presbyterian Hospital, said the approach could fill a major gap in cardiac care.
“As a clinician who opens up arteries with stents for patients who come to us with heart attacks, I am highly aware that we have a large unmet need for our patients,” said Vahl. “Too many times they are left with severe heart damage that results later in heart failure.”
Lessons from newborn hearts
The therapy builds on a biological process seen in newborn mammals. During the first few days of life their hearts briefly have the ability to regenerate damaged muscle cells.
ANP plays a key role by encouraging new blood vessel growth, reducing inflammation and limiting scar formation. In adults, ANP production drops sharply and the regenerative capacity seen in neonates largely disappears.
ANP plays a key role by encouraging new blood vessel growth, reducing inflammation and limiting scar formation.
Experiments comparing newborn and adult mice after a heart attack revealed that in newborn hearts, the gene responsible for producing ANP’s precursor increased more than 25-fold. However, in adults, it rose only about tenfold which is insufficient for meaningful regeneration. Blocking that gene in newborn mice removed much of their heart’s natural healing ability.
“The whole idea is that we learn from nature,” said Cheng. “The neonatal heart spontaneously produces more of this molecule after a heart attack. That’s probably why young hearts can regenerate themselves. The adult can’t produce a sufficient amount so we found a way to supplement this to the heart.”
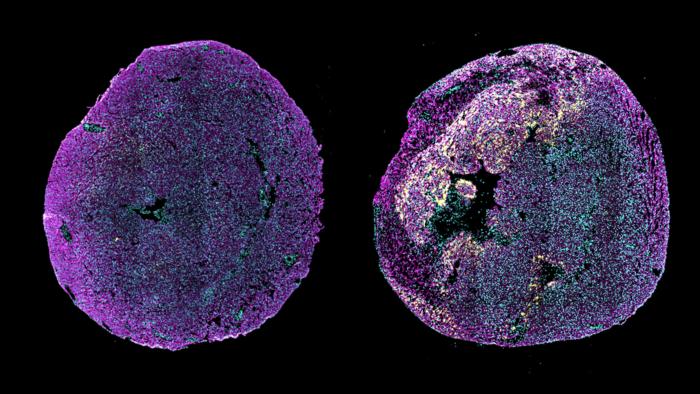

Immunofluorescence image of transverse heart sections from a healthy neonatal mouse (left) or a neonatal mouse in which myocardial infarction was induced at postnatal day 1, examined 3 days after injury (right). The yellow signal shows high levels of pro-ANP expression in the border region of the injured myocardium. Pro-ANP is an injury-responsive protein that helps promote cardiac repair in neonatal mice. Cardiomyocytes are shown in magenta (α-actinin) and cell nuclei are shown in cyan. Credit: Cheng Lab/Columbia University.
Turning muscle into a drug factory
Delivering drugs directly to the heart in a sustained and minimally invasive way has been challenging. Organs such as the liver or spleen naturally accumulate certain drugs but the heart lacks such mechanisms. Traditional approaches often involve invasive injections into the heart muscle or its blood vessels.
Delivering drugs directly to the heart in a sustained and minimally invasive way has long been a challenge.
“Because of these challenges researchers have worked on cardiac drug delivery with infusions directly into the blood vessels of the heart, injections into the heart muscle and injections into the pericardium, which is the sac surrounding the heart,” Vahl said. “All of these methods are invasive and need to be performed in a cath lab.”
The new approach uses skeletal muscle as a production site. The RNA instructs muscle cells to make pro-ANP, which travels through the bloodstream until it reaches the heart, where Corin converts it into active ANP. The therapy relies on self-amplifying RNA that replicates inside cells so the effects of a single injection lasted at least four weeks.
“The patient doesn’t have to go to the hospital today and tomorrow,” Cheng said. “They may only have to go once per month.”
Promising results and next steps
Laboratory studies showed a single injection reduced scarring and improved heart function in small and large animals, including aged mice, animals genetically prone to atherosclerosis and mice with diet-induced type 2 diabetes. The therapy remained effective even when treatment was delayed for a week after a heart attack.
“We tested the drug in different disease comorbidities and we also tested delayed treatment,” said Cheng. “We hope that, even if a patient had a heart attack weeks before getting the drug, it’s still effective.”
Cell damage is a problem that not only affects the heart but many organs.
Beyond heart attacks, the same RNA strategy could potentially treat conditions such as kidney disease, high blood pressure and preeclampsia.
“Cell damage is a problem that not only affects the heart but many organs,” said Vahl. “If we can prove that this type of therapy can regenerate cardiac cells in the clinical setting, the idea could potentially be transferred to other organs.”
Cheng hopes to manufacture the therapy at the Columbia Initiative in Cell Engineering and Therapy and begin a Phase I safety trial at Columbia University Irving Medical Center.
“We can leverage our in-house resources for manufacturing and then start a clinical trial,” said Cheng. “Columbia can do both.”